Best 4 Pec Minor Release Techniques – Pain Free And Safe Movements
Best 4 Pec Minor Release Techniques
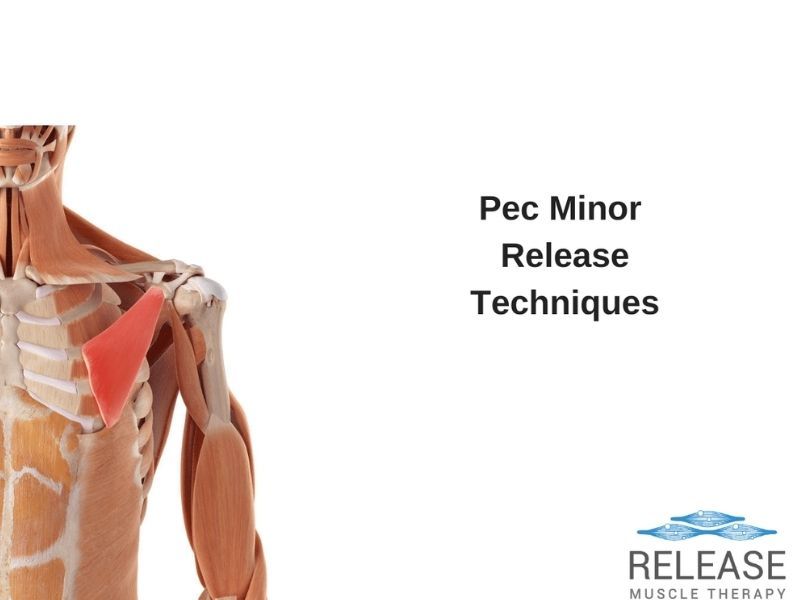
Most people are quite familiar with the larger, more superficial chest muscles, called the pectoralis major, however, underneath this muscle is another, called the pec minor. The pec minor release techniques later in this article will be specific to this muscle.
This muscle is very important to address, since it’s responsible for pulling the shoulder blade forward and down onto the ribs. (contributing to the rounded shoulders appearance).
If during an evaluation there is an upper cross syndrome with rounded shoulders and excessive forward head positioning, this muscle should be addressed.
For the most part, in any upper body impairment the pec minor is likely to be strongly involved.
Pec Minor Release w Tennis Ball
The pectoralis minor can be addressed with a tennis ball. This is one of my favorite self pec minor releases. Now, one thing to mention here is that you will NOT be making contact directly with the muscle.
Since the pectoralis major lays over the top, you’ll be influencing the pec minor indirectly with this technique. You will need to play with ball positioning to find the most tender spots.
Pec Minor Release Massage
Addressing the pec minor with massage release techniques can be very powerful and useful. My favorite position for this is side lying, as it allows for gravity assistance in moving the pec major out of the way.
However, some therapists prefer to do this supine (client laying on their back). The preference will ultimately depend on the anatomy of the individual, and the therapist’s ability to feel the muscle.
Pec Minor Stretch
The pec minor can be challenging to stretch due to how deep the muscle is and it’s function.
It’s not uncommon to feel either a stretch OR some discomfort on the front of the shoulder when attempting to stretch the pec minor. Therefore, take your time when setting up this stretch and avoid being too aggressive.
Pec Minor Release – Post Isometric Relaxation
Post-isometric relaxation is very effective for the pec minor muscles, in particular for resolving pec minor trigger points.
A therapist is needed for this technique.
Lay on your back with arms down at sides. The therapist will guide the shoulder slightly up away from the nipple as well as down toward the table. You do NOT need to go far with this stretch.
Hold for 8-10 seconds, take a deep breathe in, and exhale as you attempt to relax further into the stretch. Next, while maintaining a light stretch, gently push the shoulder into the hand of the therapist with about a 10-15% percent effort.
Hold for 10 seconds, then take a deep breath and relax fully, allowing the therapist to take up the slack and see if the stretch can be taken a bit further. Repeat 2-3 more times or until no additional range of motion is achieved.
Thanks for checking out my recommended best pec minor release techniques.
As always, no muscle should be seen as the sole contributor to any given problem. No muscle works in isolation.
It’s always best to approach muscular imbalances with a systemic approach to get the best results. That is why I developed my Posture Hacking System.